April is Sjögren’s Awareness Month, and you are not alone if you are wondering what the jolly sounding term means—it’s actually a cute sounding name for an autoimmune disease that is anything but cute— Sjögren’s syndrome, or disease, is pronounced SHOW-grins and having dry eyes and mouth are hallmarks of the condition.
As is typical of most autoimmune illnesses, one often accompanies another, and Sjögren’s syndrome is sometimes linked to other diseases in the autoimmune family like rheumatoid arthritis or lupus.
The term “autoimmune” refers to a collection of conditions where the body’s immune system attacks its own cells and tissues. In simple terms, a malfunction occurs within the body, resulting in its inability to recognize “self” cells, instead seeing cells produced by the body as invaders.
The medical field is not sure why some people develop autoimmune conditions as opposed to others, though research indicates there is a genetic component. Certain genes tend to place individuals at a higher risk for developing an autoimmune disease. One factor isolated by researchers has been dubbed the Rheumatoid Factor (RF) and is present in upwards of 40-75% of autoimmune sufferers, though its presence alone does not necessarily equal having a rheumatic disease.
Feeling dry
On the surface having dry eyes and mouth may not sound too alarming, but oh contraire, because 60-70% of our bodies are made up of water for a reason.
Water can be found in cells, bones, muscles, and organs—even found around the cells in blood and tissue. So, yeah, having hydrated eyes and mouth is pretty important.
Occurring at any age, but most often diagnosed in one’s 40s, the syndrome dries out the mucous membranes and other moisture secreting glands of the eyes and mouth. Initially, this leads to decreased tear and saliva production.
Later, the patient may develop vision issues and dental damage. A dry mouth can cause an increase in cavities, sometimes resulting in tooth loss for the patient.
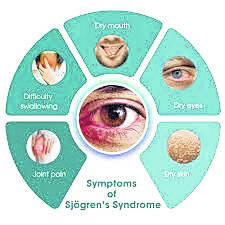
Symptoms of Sjögren’s syndrome
Sjögren’s patients have periods of remission, where they have limited to no active disease, and periods of intense disease involvement known as a “flare” and characterized by an increase in symptoms such as:
• Dry eyes that might feel itchy or like they are burning. Some patients describe a gritty feeling, as if a grain of sand is trapped inside.
• Dry mouth can make it difficult for a patient to speak or swallow. Feeling like one’s mouth is stuffed full of cotton is reported by sufferers.
• Joint pain, often accompanied with swelling and stiffness
• Swollen salivary glands, usually those located behind your jaw and in front of your ears
• Skin rashes or dry skin
• Vaginal dryness
• A persistent dry cough
• Bouts of intense fatigue
Risk factors and complications
Sjögren’s syndrome disproportionately affects women, so much so being of the female gender is considered a risk factor, along with being over the age of 40, and already having another rheumatic disease such as lupus or rheumatoid arthritis.
Common complications associated with the syndrome are an increase in dental cavities, yeast infections such as thrush, or an oral yeast infection, and vision problems like light sensitivity, blurred vision, and corneal damage.
Less often Sjögren’s syndrome is accompanied by more serious complications such as:
• Damage to lungs, kidneys or liver, resulting in inflammation causing pneumonia, bronchitis or other problems in the lungs, kidney function problems, and might even cause hepatitis or cirrhosis of the liver.
• A small percentage of Sjögren’s sufferers develop cancer of the lymph nodes, or lymphoma.
• When nerves are affected, patients report feelings of numbness, tingling and burning in their hands and feet, aka peripheral neuropathy, a condition widely known for affecting diabetics.
Diagnosing Sjögren’s
For a patient to obtain a diagnosis of Sjögren’s disease, the patient must first undergo a battery of lab tests, possible lip biopsies and eye and saliva gland assessments through tests like the Schirmer tear test or Ocular surface staining.
The Schirmer tear test measures tear production. To conduct the test, a filter paper is placed under the patient’s lower eyelid to determine the dryness of their eye.
Dyes like Rose Bengal or fluorescein are used to stain the surface of the eye with the goal of detecting the presence of corneal damage due to progression of the disease.
Additionally, salivary gland imaging may also be conducted using sialography, or an X-ray using dye to highlight saliva and gland functioning within the mouth.
A constant when diagnosing most, if not all, autoimmune diseases is lab work.
When diagnosing Sjögren’s disease, the presence of autoantibodies is essential.
Typical lab tests for Sjögren’s, and most autoimmune conditions,include testing for Anti-Ro/SSA antibodies [found in roughly 60-80% of patients and are highly indicative of the presence of Sjögren’s], Anti-La/SSB antibodies [found in 30-50% of Sjögren’s patients], Antinuclear Antibody (ANA) [positive in 80% of patients], and Rheumatoid factor or RF [detected in 40-75% of autoimmune patients].
Simply having a positive ANA result is not where the ANA test ends. Once the presence of antibodies is detected, lab technicians determine the pattern of the cells—a speckled or homogeneous pattern is most often associated with a diagnosis of Sjögren’s.
Outlook
There is no cure for autoimmune disease, and there is no cure currently known for treating Sjögren’s disease. Consequently, treatment for the condition focuses on prevention, maintenance, and flare treatment.
Leave a Reply
You must be logged in to post a comment.